The field of healthcare is diverse and dynamic, encompassing a wide range of roles that contribute to patient care and well-being. Two integral roles within this realm are Registered Nurses (RNs) and Nurse Practitioners (NPs). While both of these professionals play essential roles in delivering high-quality healthcare services, they have distinct differences in terms of education, scope of practice, responsibilities, and specialization. Understanding these differences between registered nurses and nurse practitioners is crucial for anyone considering a career in nursing or seeking healthcare services.
Education and training
Registered Nurses (RNs) education
Registered Nurses embark on their journey with diverse educational pathways. These routes include obtaining a diploma, associate’s degree in nursing (ADN), or a bachelor of science in nursing (BSN) degree. These educational routes equip RNs with a foundational understanding of nursing practices, patient care techniques, and medical procedures. Successful completion of the NCLEX-RN examination marks the culmination of their education, opening the door to practicing as a licensed registered nurse.
Nurse Practitioners (NPs) education
Nurse Practitioners, on the other hand, undertake a more advanced educational trajectory. A Master of Science in Nursing (MSN) or Doctor of Nursing Practice (DNP) degree is the cornerstone of their preparation. These programs are intensive, blending specialized coursework with hands-on clinical training. This higher education arms NPs with a deeper comprehension of intricate medical conditions, an array of treatment modalities, and adept patient management strategies.
Scope of practice
Registered Nurses (RNs) scope
Registered Nurses function within the context of a collaborative healthcare ecosystem. Under the guidance of physicians and nurse managers, they excel at tasks such as medication administration, wound care, and vigilant patient monitoring. As essential team players, RNs execute tasks that are directed by healthcare providers, ensuring seamless patient care delivery.
Nurse Practitioners (NPs) scope
Nurse Practitioners, as a result of their advanced education, enjoy an expanded scope of practice. NPs possess the authority to independently diagnose and treat illnesses, order diagnostic tests, prescribe medications, and develop comprehensive treatment plans. This autonomy is particularly valuable in regions with limited physician accessibility, as NPs can bridge the healthcare gap effectively.
Job responsibilities
Registered Nurses (RNs) responsibilities
The role of a Registered Nurse is characterized by hands-on patient care and assisting in medical procedures. Beyond these tasks, RNs shoulder the responsibility of ensuring patient comfort, effective communication, and acting as staunch advocates for their patients’ needs. Collaborating with a multidisciplinary healthcare team, they facilitate cohesive patient care journeys.
- Direct patient Care: Providing hands-on care, administering treatments, and monitoring patients’ conditions.
- Assistance in procedures: Assisting with medical procedures, wound care, and medication administration.
- Patient advocacy: Advocating for patient needs and concerns within the healthcare team.
- Collaboration: Working closely with physicians, nurses, and other healthcare professionals.
- Care plans: Implementing and following care plans to ensure patients’ well-being.
Nurse Practitioners (NPs) responsibilities
Nurse Practitioners are distinguished by their capacity for comprehensive patient management. Their skill set encompasses holistic patient assessments, precise diagnoses, and the formulation of tailored treatment plans. A defining aspect of NP practice is their dedication to health promotion, disease prevention, and the invaluable time they invest in patient education. This commitment to patient empowerment underscores their role as educators and caregivers.
- Diagnoses and treatment: Independently diagnosing medical conditions and developing tailored treatment plans.
- Comprehensive assessments: Conducting thorough patient assessments, considering holistic health aspects.
- Prescribing authority: Prescribing medications and ordering necessary diagnostic tests.
- Health education: Educating patients about diagnoses, treatment options, and preventive measures.
- Autonomy: Operating with a higher level of independence in patient care decisions.
Specialization
Registered Nurses (RNs) specialties
Registered Nurses have the latitude to specialize in various branches of healthcare. Pediatric nursing, critical care, oncology nursing, and more are avenues through which RNs can channel their expertise. These specializations enable them to cultivate in-depth knowledge about specific medical conditions and patient demographics.
- Pediatric Nursing
- Critical Care Nursing
- Oncology Nursing
- Obstetric and Maternity Nursing
- Emergency Room Nursing
- Surgical Nursing
- Psychiatric Nursing
- Geriatric Nursing
Nurse Practitioners (NPs) specializations
Nurse Practitioners, building upon their advanced education, can embark on diverse specialized paths. The spectrum of NP specializations includes family practice, adult gerontology, pediatrics, women’s health, psychiatric-mental health, and more. This capability to specialize further bolsters their role as primary healthcare providers for specific patient populations.
- Family Nurse Practitioner
- Adult-Gerontology Nurse Practitioner
- Pediatric Nurse Practitioner
- Women’s Health Nurse Practitioner
- Psychiatric-Mental Health Nurse Practitioner
- Acute Care Nurse Practitioner
- Neonatal Nurse Practitioner
- Oncology Nurse Practitioner
Collaboration and autonomy
Registered Nurses (RNs) collaboration
The hallmark of Registered Nurses’ role lies in collaboration. Working in tandem with physicians, nurse managers, and fellow nurses, RNs execute care plans, assist in medical procedures, and contribute to the seamless functioning of the healthcare team. Their communication and coordination skills are pivotal in optimizing patient outcomes.
Nurse Practitioners (NPs) autonomy
Nurse Practitioners navigate the healthcare landscape with a higher degree of autonomy. This autonomy extends to making independent decisions in patient care, though collaboration with physicians remains essential for complex cases. NPs often serve as primary care providers, particularly in contexts where their specialized knowledge and skills are the cornerstone of effective healthcare delivery.
Continuing education
Registered Nurses (RNs) education
For Registered Nurses, the pursuit of continuing education is a gateway to career advancement and specialization. By pursuing bachelor’s or master’s degrees, RNs can deepen their skills and expand their horizons. These opportunities facilitate professional development, enabling them to assume roles such as clinical nurse specialists or nurse educators.
Nurse Practitioners (NPs) continuing education
The dynamic nature of healthcare necessitates continuous learning for Nurse Practitioners. Evolving medical knowledge prompts NPs to stay abreast of new treatment protocols, guidelines, and best practices. Maintaining certifications and licensure ensures that NPs remain at the forefront of healthcare excellence.
Patient interaction
Registered Nurses (RNs) patient interaction
The essence of a Registered Nurse’s role is centered around direct patient interaction. Beyond providing hands-on care, RNs act as empathetic listeners and educators. Patient education is a key facet, where RNs impart knowledge about treatment plans, self-care practices, and health maintenance.
Nurse Practitioners (NPs) patient interaction
Nurse Practitioners take patient interaction to a holistic level. They not only diagnose and treat medical conditions but also emphasize educating patients about their diagnoses, treatment options, and lifestyle modifications. This approach nurtures a patient-provider partnership grounded in trust and empowerment.
Complex cases and referrals
Registered Nurses (RNs) cases
Registered Nurses are adept at handling routine patient care and emergencies alike. In cases where complexity escalates, RNs are quick to identify the need for physician intervention. Ensuring patient safety, they facilitate seamless patient transfers and maintain open lines of communication within the healthcare team.
Nurse Practitioners (NPs) cases
Nurse Practitioners thrive in managing an extensive array of medical conditions. Their advanced training enables them to independently diagnose and treat complex cases. For intricate scenarios that warrant specialized expertise, NPs collaborate with specialists to ensure comprehensive patient care.
Legal and regulatory differences
Registered Nurses (RNs) regulation
Registered Nurses operate within the framework outlined by nursing boards and regulatory bodies. They follow physician orders and care plans diligently, adhering to ethical and legal standards that govern nursing practice. These regulations ensure consistent and high-quality patient care.
Nurse Practitioners (NPs) regulation
Nurse Practitioners’ practice is subject to state-specific regulations that dictate their level of autonomy. While some states grant NPs full practice authority, others impose restrictions that influence their scope of practice. This variance in regulation underscores the importance of understanding state laws and acting within their confines.
Income and salary
Registered Nurses (RNs) income
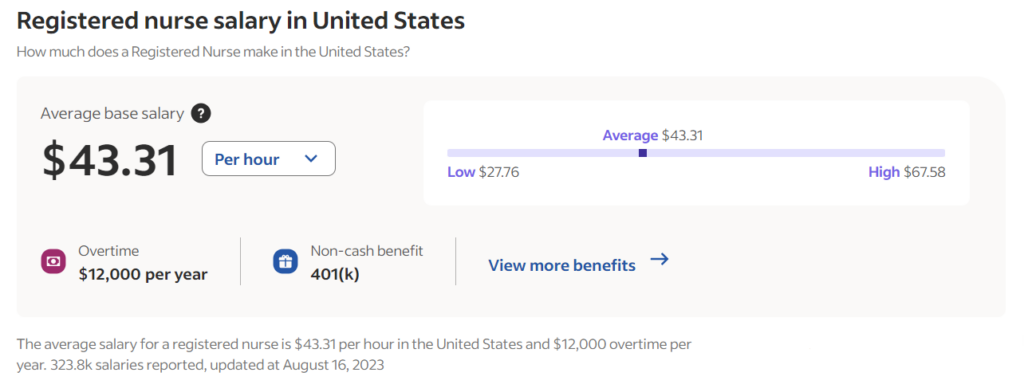
Registered Nurses’ income is a reflection of factors such as education, experience, and specialization. Their earnings range from moderate to competitive and opportunities for salary growth can be seized by pursuing advanced degrees and venturing into specialized roles. As the experience increases from year to year, the salary range for RNs also goes higher.
As of the latest available data, the average annual salary for Registered Nurses in the United States is around $92,430 (approximately $43.31 per hour).
Nurse Practitioners (NPs) salary
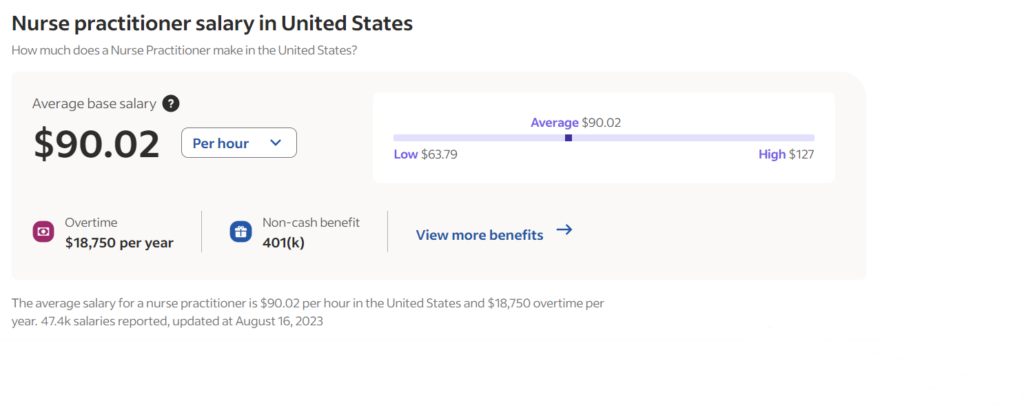
Nurse Practitioners, given their advanced education and expanded responsibilities, generally command a higher salary compared to RNs. Their compensation is a testament to their specialized skills and contributions to patient care. The variation in salary is influenced by factors such as specialization, geographical location, and years of experience. For instance, states like California, New York, and Massachusetts tend to offer higher NP salaries due to the higher cost of living and demand for healthcare services.
An NP can earn an average of $121,183 per year in the USA as per Indeed salary data. This can be rounded to $90.02 per hour.
Certifications
Registered Nurse (RN) certifications
- Basic Life Support (BLS): CPR and emergency response training.
- Advanced Cardiovascular Life Support (ACLS): Critical care cardiac life support training.
- Pediatric Advanced Life Support (PALS): Pediatric emergency care training.
- Medical-Surgical Certification: Expertise in medical-surgical nursing.
- Critical Care Nursing Certification: Specialization in critical care patient management.
- Oncology Certified Nurse (OCN): Specialized knowledge in oncology nursing.
- Certified Pediatric Nurse (CPN): Expertise in pediatric patient care.
- Certified Emergency Nurse (CEN): Specialization in emergency department care.
- Certified Dialysis Nurse (CDN): Expertise in dialysis patient care.
Nurse Practitioner (NP) Certifications
- Family Nurse Practitioner (FNP-BC): Specialization in family-centered care.
- Adult-Gerontology Nurse Practitioner (AGNP-BC): Expertise in adult and geriatric care.
- Pediatric Nurse Practitioner (PNP-BC): Specialization in pediatric care.
- Women’s Health Nurse Practitioner (WHNP-BC): Focus on women’s health issues.
- Psychiatric-Mental Health Nurse Practitioner (PMHNP-BC): Expertise in mental health care.
- Acute Care Nurse Practitioner (ACNP-BC): Specialization in acute care settings.
- Certified Nurse Midwife (CNM): Focus on prenatal, childbirth, and postpartum care.
- Certified Registered Nurse Anesthetist (CRNA): Expertise in anesthesia administration.
- Adult-Gerontology Acute Care Nurse Practitioner (AGACNP-BC): Expertise in acute care for adults and older adults.
Career advancement
Registered Nurses (RNs) advancement
Registered Nurses are not confined to a single career trajectory. Opportunities abound for RNs to ascend the career ladder, transitioning into leadership, management, or education roles. Pursuing graduate degrees paves the way for broader career prospects, enabling them to become clinical nurse specialists or nurse educators.
Nurse Practitioners (NPs) career progression
For Nurse Practitioners, career progression takes multifaceted forms. They can choose to specialize further within the realm of NP practice, honing their expertise in specific areas. Additionally, NPs can transition into advanced practice fields, where their specialized skills contribute to pioneering research and policy development.
Contribution to healthcare system
Registered Nurses (RNs) contribution
The healthcare system relies heavily on the contributions of Registered Nurses. Their involvement spans direct patient care, support for physicians, and ensuring patient safety and comfort. As the linchpin of the healthcare team, RNs sustain the smooth operation of healthcare facilities.
Nurse Practitioners (NPs) impact
Nurse Practitioners wield their expertise as a potent tool to address healthcare disparities. In regions with limited access to physicians, NPs step in to provide vital primary care and preventive services. Their dedication translates to improved patient access, enhanced health outcomes, and an overall positive impact on community health.
How to step up from RN to NP
Elevating your career from a Registered Nurse (RN) to a Nurse Practitioner (NP) involves a strategic pathway of educational and professional growth. Start by pursuing an advanced degree, such as a Master of Science in Nursing (MSN) or a Doctor of Nursing Practice (DNP), which equips you with the advanced knowledge and skills necessary for NP practice. Gain valuable clinical experience in your chosen specialty area as an RN, honing your expertise and understanding of patient care nuances. Successfully passing the NP certification exam is the final step, granting you the autonomy to diagnose, treat, and manage patients independently.
Conclusion
In summary, the distinctions between Registered Nurses and Nurse Practitioners are rooted in education, scope of practice, responsibilities, and specialization. While Registered Nurses play a vital role in healthcare by providing direct patient care and assisting with medical procedures, Nurse Practitioners bring an advanced level of education and training to the table. NPs can diagnose and treat medical conditions, prescribe medications, and develop treatment plans, making them an integral part of the healthcare team, especially in areas with limited physician access. Both roles contribute significantly to the healthcare system, working together to ensure the well-being and quality of life for patients across the globe.


